
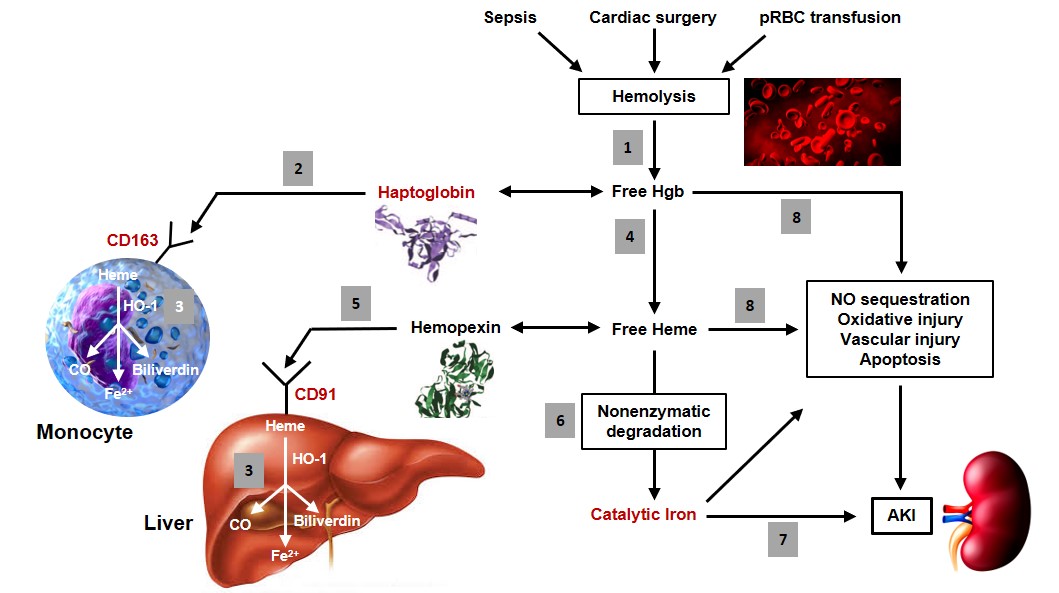
Overview of catalytic iron-induced acute kidney injury (AKI). 1: Hemolysis, which can occur through endogenous or exogenous processes, results in the release of free hemoglobin (Hgb) into the plasma. 2: Free Hgb is bound by haptoglobin and the complex is taken up by monocytes and macrophages via the scavenger receptor, CD163. 3: Once internalized, Hgb is broken down into heme, which is degraded further by heme oxygenase-1 (HO-1) into carbon monoxide (CO), biliverdin, and Fe2+. The latter is oxidized into Fe3+ and sequestered by ferritin, which is upregulated by HO-1. 4: Free Hgb not sequestered by haptoglobin may be oxidized into free heme in the circulation. 5: Free heme is sequestered by hemopexin and taken up by hepatocytes, vascular smooth muscle cells, and other cell types via the scavenger receptor, CD91. 6: When the ability of haptoglobin and hemopexin to scavenge free Hgb and free heme is overwhelmed, respectively, nonenzymatic degradation (i.e., in the absence of HO-1) may release catalytic iron from heme. 7: This catalytic iron catalyzes the formation of free radicals, which can damage macromolecular components of cells, resulting in AKI. 8: Even in the absence of catalytic iron generation, free Hgb and free heme may contribute to AKI by a variety of mechanisms including: nitric oxide (NO) sequestration, which results in vasoconstriction; oxidant-mediated cellular damage; vascular injury; and induction of apoptosis. Key targets for potential therapeutic intervention are colored in red.

CLINICAL TRIALS
We are conducting DEFEAT-AKI (Deferoxamine for the Prevention of Acute Kidney Injury), an NIH-funded, phase 2, multicenter, double-blind, placebo-controlled, randomized clinical trial investigating whether intraoperative iron chelation with IV deferoxamine reduces the incidence of postoperative AKI in high risk adult patients undergoing cardiac surgery. Additional info can be found here.

BIOMARKER STUDIES
Catalytic iron, also known as non-transferrin-bound iron, plays a key role in the pathogenesis of AKI in animal models. We established that plasma catalytic iron levels are elevated in patients with AKI and are associated with increased hospital mortality, need for renal replacement therapy, and death.

GENETICS STUDIES
Heme oxygenase-1 (HO-1), the rate limiting enzyme in the degradation of heme, has important anti-inflammatory and cytoprotective effects in the kidneys and elsewhere. We established that a common polymorphism in the HO-1 gene is associated with AKI following cardiac surgery.
SELECTED PAPERS FROM OUR RESEARCH
Sharma S, Leaf DE. Iron Chelation as a Potential Therapeutic Strategy for AKI Prevention. J Am Soc Nephrol 2019;30(11):2060-2071. Pubmed
Leaf DE, Rajapurkar M, Lele SS, Mukhopadhyay B, Boerger EAS, Mc Causland FR, Eisenga MF, Singh K, Babitt JL, Kellum JA, Palevsky PM, Christov M, Waikar SS. Iron, Hepcidin, and Death in Human Acute Kidney Injury. J Am Soc Nephrol 2019;30(3):493-504. Pubmed
Leaf DE and Swinkels DW. Catalytic Iron and Acute Kidney Injury. Am J Physiol Renal Physiol 2016;311(5):F871-6. PubMed
Leaf DE, Body, SC, Muehlschlegel JD, McMahon GM, Lichtner P, Collard CD, Shernan SK, Fox AA, Waikar SS. Length Polymorphisms in Heme Oxygenase-1 and Risk of AKI following Cardiac Surgery. J Am Soc Nephrol 2016;27(11):3291-97. PubMed
Leaf DE, Rajapurkar M, Lele SS, Mukhopadhyay B, Rawn J, Frendl G, Waikar SS. Increased plasma catalytic iron in patients may mediate acute kidney injury and death following Cardiac Surgery. Kidney Int 2015;87(5):1046-54. PubMed
Leaf DE, Rajapurkar M, Lele SS, Mukhopadhyay B, Waikar SS. Plasma Catalytic Iron, AKI, and Death among Critically Ill Patients. Clin J Am Soc Nephrol 2014;9(11):1849-56. PubMed
